August 5, 2021 | Peter Corless
August 5, 2021 | Peter Corless
.jpg?width=873&name=A%20Growing%20Number%20Of%20Organizations%20%26%20Associations%20Join%20The%20Vaccine%20Mandate%20Movement%20%20(1).jpg) There have been several developments this past week on the vaccine mandate front. Dozens of organizations have instituted mandates, and a growing list of industry associations are offering their support for doing so. Could this momentum mean we’re headed toward a federal mandate for healthcare workers? Only time will tell.
There have been several developments this past week on the vaccine mandate front. Dozens of organizations have instituted mandates, and a growing list of industry associations are offering their support for doing so. Could this momentum mean we’re headed toward a federal mandate for healthcare workers? Only time will tell.
Let’s take a look at where staff vaccination rates stand today, which organizations and associations are implementing and supporting mandates, and the implications of it all on the workforce.
Vaccine Acceptance Rises Sharply & Then Levels Off
As of July 25, 2021, CMS data showed that only 59% of staff in nursing homes and long-term care facilities nationwide were partially or fully vaccinated. While that number has steadily grown since December of 2020, when OnShift research found that only 32% were planning to take the vaccine when it became available, we have not met the industry’s goal of 75%. Long-term care and assisted living facilities are still fighting the virus, especially the highly transmissible Delta variant.
To be clear, this lower-than-hoped-for vaccine participation rate is through no fault of post-acute care organizations, who have done their due diligence to increase employee vaccine acceptance through education and one-on-ones with hesitant staff members. Some examples of these efforts include establishing regular educational sessions, open office hours and vaccine resource lines to answer questions, dispel misinformation and help staff make an informed decision. Other organizations offered cash incentives, entered participating team members in drawings and drummed up creative campaigns with the help of local celebrities. One even distributed a video of their CEO receiving and endorsing the vaccine to all staff members.
As a result of these initiatives, nearly half of employees that took OnShift’s vaccine acceptance survey in March of this year said that they were satisfied or very satisfied with their organization’s education efforts. And these efforts contributed to a 94% increase in willingness to take the vaccine from our initial survey the previous year.
Still, as the Delta variant has picked up steam across the US, it’s become clear that while education is important, we are simply running out of time.
Senior Care Organizations Introduce Mandates; Associations & Affiliates Stand In Solidarity
“The ‘why’ is so incredibly simple: Vaccines make our residents as safe as possible,” Randy Bury, CEO of Good Samaritan Society said regarding their recent mandate as a condition of employment. “Frankly, I’m tired of the time, the effort and the attention we constantly have to put into this conversation. If everyone were vaccinated, this thing would be over by now.”
This is backed up by another set of statistics recently released by AHCA. The graph below vividly displays there is a clear correlation between staff vaccine rates and resident COVID-19 cases and deaths.
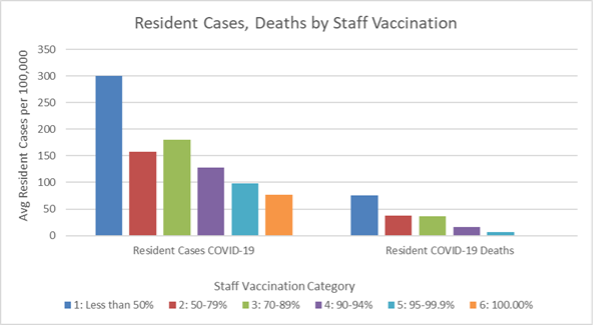
*Data shared by AHCA
And over the past couple weeks, we’ve seen an uptick in others following suit. Just a couple days ago, Genesis HealthCare, the nation’s largest skilled nursing provider, announced their mandate.
Genesis CEO Harry Wilson said of the organization’s decision: “Despite vaccination rates above the national average, the growing spread of the Delta variant makes clear that we need to increase our vaccination rates substantially to better protect our patients, residents and employees.”
Individual states are coming out with their own mandate action plans, like New Jersey, which will implement a statewide mandate for all health workers, including those in senior care, if the vaccination rates do not improve by Sept. 7. The mandate requires that workers be vaccinated or be subject to frequent testing. Gov. Phil Murphy further warned, “If we do not see significant increases in vaccination rates among the employees in these settings, we are ready and willing to require all staff to be vaccinated as a condition of their employment.”
Massachusetts Gov. Charlie Baker put his foot down when he announced yesterday that the state’s long-term care staff must be vaccinated by Oct. 10. Skilled Nursing News reported, “Massachusetts appears to be the first state to issue a COVID-19 vaccine mandate for nursing facility workers, according to the state’s long-term care association.”
Organizations and associations are standing up to support providers mandating the vaccine. Most recently, AHCA/NCAL and LeadingAge joined the list of over 56 other professional healthcare groups endorsing providers making this difficult decision. AHCA also recently published compelling data that shows facilities with high staff vaccination rates also have a higher census.
-1.png?width=600&name=Untitled%20design%20(1)-1.png)
*Data shared by AHCA
The Implications Of The Vaccine Mandate On The Workforce
James M. Berklan reports for McKnight’s Long-Term Care News, “The endorsement of a vaccination mandate is seen as a bold move, especially in long-term care, where critics say ongoing staffing shortages would be exacerbated if nurses and other workers decide to quit or stay away from work rather than become vaccinated.”
The fear of a mass exodus was likely what has made many providers hesitant to require staff take the vaccine, which is completely understandable. The CNA turnover rate reached 129% in March and competition in the labor market is at an all-time high. If employees were to leave due to a vaccine mandate, who would they replace them with? I like Bury’s outlook on the situation.
“The biggest concern right away is staffing. You keep hearing, ‘What if they leave you?’ and all that boogeyman stuff,” he told McKnight’s Long-Term Care News. “But there’s a flip side to that, and I’ve seen it in my emails this week. There’s vaccinated staff who are very, very happy that we’re mandating this so they don’t have to worry about being the next breakthrough case or taking the virus home to their kids.”
And what about replacing any staff members that choose to leave? Bury points to the mandates as a potential differentiator to attract future workers.
“The last thing we want to do is lose any staff member over this,” he said. “But it’s not only about people who already work for us. It’s people contemplating their next job, or just coming out of college. We actually think it will be an attraction for them.”
All in all, resident and staff safety is a priority for LTC and senior living organizations. That’s why mandating the vaccine for senior care employees is gaining traction and support. I sympathize with all of the providers grappling with this difficult decision, but I do believe that Bury’s theory has legs. Mandating the vaccine will provide peace of mind for existing vaccinated staff and position organizations as safe environments dedicated to serving and protecting our nation’s elderly.
Subscribe to the OnShift Blog
Recent Posts
Categories
About Peter Corless
Peter Corless is Executive Vice President of Enterprise Development for OnShift. Peter is a recognized HR leader in post-acute care and is well-known for his achievements at some of the country’s largest post-acute care organizations, including Kindred Healthcare and Genesis HealthCare. As an experienced, chief administrative and human resources officer within these organizations, he developed strategies that reduced turnover, improved recruiting and hiring strategies, and reduced labor costs.
See for yourself why thousands of providers rely on OnShift’s innovative software for recruitment, hiring, workforce management, pay and engagement. Request your personalized demo today.